This was 2020.
The year of Covid-19
Part IV
Wave after wave
Covid’s comeback
After enduring a near-seven week lockdown, New Zealand eventually settled into a comfortable lull.
The country had all but eliminated the virus by May, and had been in alert level 1 since June 8, when health authorities announced the last remaining active case, linked to the CHT St Margaret’s rest home cluster in Auckland, had recovered.
Against the odds, as winter closed in the country was Covid-19 free for the first time since February 28.

New Zealand had more than 100 days of freedom at alert level 1. Then new community cases were confirmed, seemingly out of nowhere. Hagen Hopkins/Getty
On August 9, a Sunday just shy of six months since the first case was confirmed, New Zealand marked 100 days without community transmission of the virus – joining a handful of countries, many much smaller and more remote than New Zealand, to achieve such a feat.
Headlines celebrating New Zealand’s success were splashed across local and international media outlets, while the country basked in its own glory at achieving such a milestone.
But a surprise 9:15pm press conference just 48 hours later was a jarring reminder of the insidiousness of Covid-19, raging outside our borders.
An Auckland family of four, with no known link to overseas travel, had tested positive for the virus, it was announced on August 11.
Little more than 12 hours later, at noon the next day, Auckland was moved to alert level 3 and the rest of New Zealand was raised to alert level 2 as authorities rushed to contain the outbreak.
The country’s largest city was cut-off, with police checkpoints lining the regional borders.

A surprise press conference late on a Tuesday saw Auckland plunge back into level 3 lockdown for more than a month. Monique Ford/Stuff
The spate of cases ballooned to the country’s largest cluster, with 179 cases linked to it, and led to three further deaths. These included distinguished physician and former Cook Islands prime minister Dr Joe Williams, and brothers Nigel and Alan Te Hiko, who died aged 54 and 58, respectively, just two weeks apart.
The outbreak also thrust South Auckland into the spotlight as an unwilling protagonist – bringing along with it a barrage of online hate directed at the area and the Pasifika community.
While the country has so far avoided another upswing through alert levels as a result of new community cases, there have been a number of incursions emerging from issues at the border - including one which led to the August cluster.
Two other outbreaks, including one from a returnee infected in a quarantine facility and the latest from port workers infected by incoming seafarers, were controlled at an early stage. The others involved infections of border facility workers: health workers on two occasions and a maintenance worker.

Professor Michael Baker says New Zealand is stressing its border defences with the large number of Kiwis returning, prompting him to propose a different approach. Supplied
Epidemiologist Dr Michael Baker, from the University of Otago, says it was always inevitable we would see a resurgence of Covid-19 in New Zealand, so long as we’re in a world where the virus is circulating.
The SARS-CoV-2 virus is likely to infect most people on the planet, he says, largely because it got the balance “exceptionally right” for transmission.
However, the events at the border were regarded as system failures by Baker and fellow Otago University expert, Associate Professor Nick Wilson, who called for a review and shake-up of the managed isolation and quarantine processes.
They say the goal should be to have complete containment of infection at the border and no cases in the community.
Baker says elimination remains the right goal, and New Zealand remains on the right track with “very good” systems in place to support this. But this is in conflict with factors making it difficult to guarantee “long-term” success.
They say the use of hotels for quarantine - for which they are not designed - and poor system design, including a lack of testing for seafarers flying into the country to join their ships, were contributing factors in issues at the border.
A similar border breach brought Melbourne to a screeching halt in July, sending the state back into a six-week lockdown in the chill of winter. Daily infection numbers peaked at 723.

Bourke St, in Melbourne’s beating heart, resembled a ghost-town as it went back into lockdown in July. Quinn Rooney/Getty Images
Infections that began in quarantine hotels were later confirmed as the source of the state’s deadly wave, which prompted an 8pm to 5am curfew and a “state of disaster” enforced in metropolitan Melbourne while dozens were dying.
While New Zealand has so far avoided such calamity arising from the border, the warning remains that it could happen again - prompting Baker and Wilson to propose a ‘traffic-light’ risk assessment scale for those returning to the country.
The pandemic is intensifying around the world, and it will be months before that changes, Baker says.
“We are really stressing our system with a huge number of infected people coming back, and that number will probably rise.”
Baker, alongside Wilson, has urged authorities to move from a one-size-fits-all approach to a risk-based system, allowing those from Covid-free countries to enter the country without quarantine if some controls remain in place, such as rapid testing, digital tracking and a bond payment.

New Zealand’s border defences, including the use of managed isolation and quarantine facilities, is critical in keeping Covid-19 out of the community. Michael Dawson/Supplied
The tension between what is within an individual’s control - our attitudes and actions - and the role of governments in ensuring people are protected, has been a source of much greater angst overseas.
As the days grew longer and warmer in the Northern Hemisphere, a World Health Organisation official described the pandemic as “one big wave” – warning against complacency over the summer months.
During a virtual briefing from Geneva in July, WHO’s Dr Margaret Harris stated the infection did not share influenza’s tendency to follow seasons, and urged vigilance about mass gatherings.
“We are in the first wave. It’s going to be one big wave. It’s going to go up and down a bit. The best thing is to flatten it and turn it into something lapping at your feet,” she said at the time.
The wave did not flatten. Instead, in wealthy countries such as the United Kingdom and United States it only gained momentum – growing bigger and stronger.
Daily new cases through April were over 4000 in the UK, the first peak of the pandemic in the country.
As the season changed from spring to summer, coronavirus infections fell sharply, dropping to hundreds through much of July and August.
By October, however, case numbers jumped to the tens of thousands per day. and remained consistently high drawing closer to Christmas.
In December, the number of deaths started to climb again and show no sign of slowing down, adding to a death toll that has already surpassed 60,000.
Speaking to BBC Scotland in October, UK Prime Minister Boris Johnson blamed a surge in cases on members of the public becoming “blase about transmission” in the summer months.
“We came together as a country, we got the numbers down and I’m afraid some of the muscle memory has faded,” Johnson said, as cases again rose exponentially.
Other countries suffered through similar trajectories.
In early May, the United States was reporting more than 30,000 new cases each day . As the month progressed and daily new cases decreased to around 20,000, states began relaxing their rules.
This inevitably led to cases spiking again over the summer. In June, new daily case numbers crept back up to 40,000, then 50,000 and nudging towards 60,000. On July 16 - about midway through the northern summer - daily new case numbers reached 75,000.
The number of new cases settled somewhat between August to mid-October, but the country was setting and breaking records for new case numbers on a daily basis in the lead-up to Christmas, with 205,000 new cases recorded on November 27.
By December, more than a million new cases were being recorded in the US most weeks.
More than 15 million cases of Covid-19 have been confirmed in the United States. Prior to Christmas, the country was on track to surpass 300,000 lives lost to the pandemic.
But Baker says these surges can’t solely be put down to waning compliance. He says the buck stops with those in charge.
“In the end, what we’re seeing is a consequence of Government decision-making.”
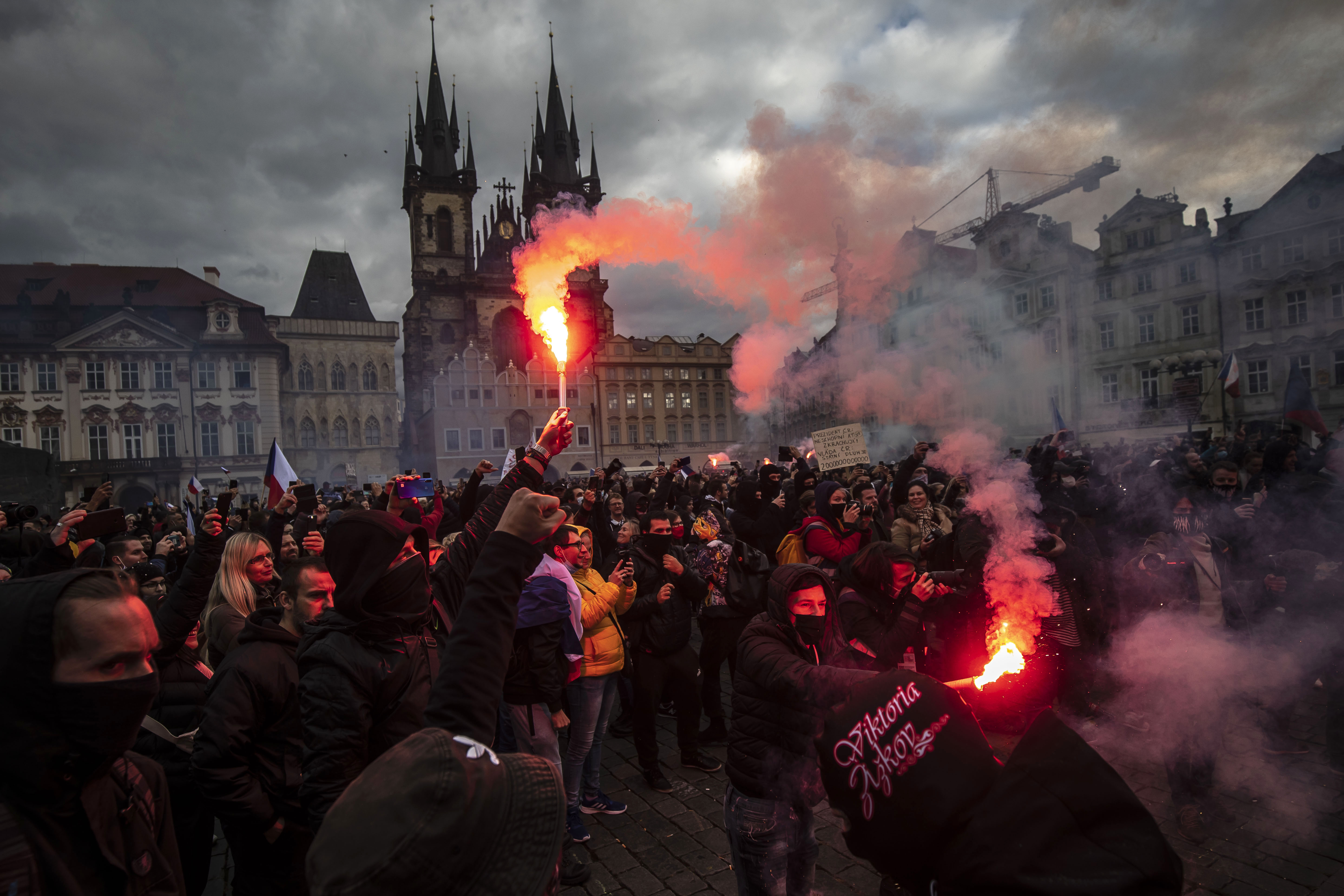
Crowds protest against Covid-19 restrictions in Prague, Czech Republic in October. Gabriel Kuchta/Getty Images
An effective pandemic response depends on things individuals do not have control over, Baker says: managing borders, and having lockdowns which are sustainable.
“There is a component of individual behaviour, but it’s hard for everyone to do the right thing in a system which I think has the wrong overall settings.”
Governments that have been “very rigid” in their response - or lack of - are now pinning their hopes on a vaccine as the way out, Baker says.
Meanwhile, citizens grapple with ‘lockdown fatigue’, becoming disenchanted with ever-changing or unclear advice.
Gabriel Kuchta/Getty Images
Fresh restrictions in several European countries in late October and early November, were met with resistance, sparking protests.
Italy, one of the hardest-hit countries in the EU, was the scene of violent protests as cinemas and theatres were shuttered, and bars and restaurants were ordered to close at 6pm.
Protestors hurling Molotov cocktails and bottles clashed with riot officers firing teargas.
While New Zealand locked down to eliminate the virus, others wanted to get to what they deemed a manageable level of cases, microbiologist Dr Siouxsie Wiles says.
But if Covid-19 is circulating at all, releasing restrictions and allowing people to move about again will inevitably give rise to new cases cropping up.
During the Northern Hemisphere spring, the US and UK put restrictions in place, “but they didn’t use that time to put in place the measures that would’ve helped them [longer term],” Wiles says.
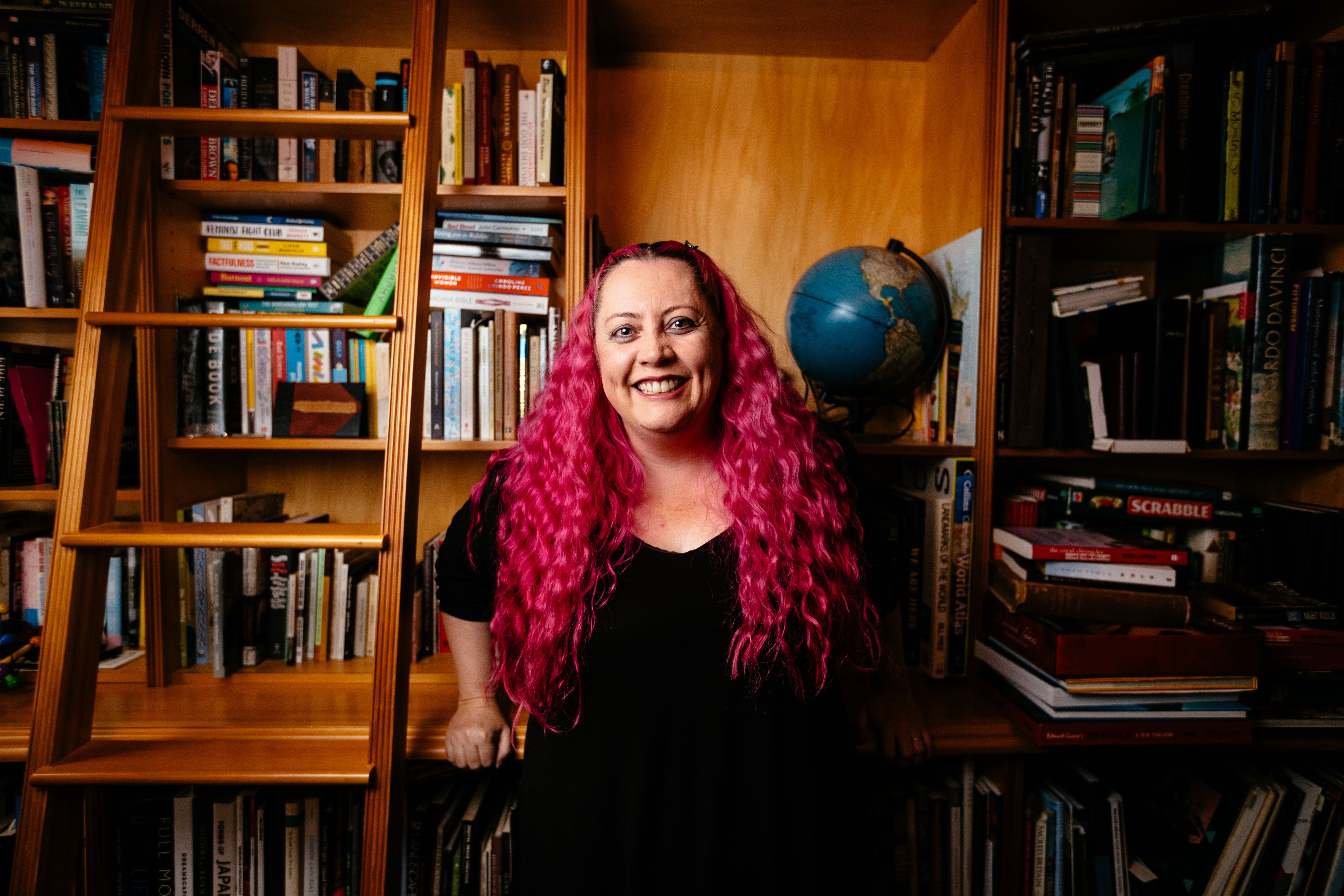
Dr Siouxsie Wiles says the pandemic should be a wake-up call. Abigail Dougherty/Stuff
As a result, health systems are struggling to cope and some hospitals are overwhelmed. Large populations are struggling through a “very difficult” winter.
By and large, those hardest hit by Covid-19 are people living in precarious conditions, with unsecure jobs or who have had to go to work through the pandemic. Being able to stay home was a privilege many didn’t have, Wiles says.
That’s what makes her angry: “It didn’t need to be this way”.
She says the pandemic has both shone a “staggering” light on “so many things wrong with society”, and presented an opportunity to change this.
“If this isn’t the wake-up call we need, I don't know what is, frankly.”


